Grant Schofield, Professor of Public Health at Auckland University says we need to exit lockdown.
Yesterday morning my teenage boys Sam and Jackson were out riding their bikes. The police pulled them over to question them about what they were doing and where they were going. They explained they were cycling for exercise and staying local. That seemed OK, but they then were told that they were sweating and sweating was dangerous, because it could transmit the virus, so they should avoid that. Wrong of course, but wow, unprecedented police powers that are beyond what New Zealanders have ever seen outside of wartime.
All in the name of eradicating Covid-19. Unite against Covid-19!
So can we achieve this?
The simple answer is no. We could with better tools. But now no.
Director-General of Health, Dr Ashley Bloomfield, recently said there is no plan B. The plan is the plan. In fact, there is strong social pressure to say nothing negative about the war effort. Negative is usually defined as anything off script, no matter how scientific. Look at my colleague Dr Simon Thornley in the last few days questioning the data being used to make our big decisions.
Back to eradication.
To eradicate this virus first, we need to know who has it, with certainty. At the most basic level that would mean that we can know if our elimination has worked. It also allows us to quarantine those who do have it, including all the asymptomatic, so they can’t unknowingly infect others. We would also be able to send those infected and now immune back out into the world.
To know these numbers we need a near-perfect test. One which correctly identifies all those who are infected, or not infected. Any false negatives, those who in reality are sick, but are tested and released as fine, would be particularly problematic. You’d also want to test on a scale with large numbers randomly across the population. That’s the only way you can confidently rule out the existence of the virus.
How does our testing go under this scientific scrutiny?
The best available test is Real Time PCR. A sequence of biochemistry allows for the detection of virus RNA. If you have these you almost certainly have Covid-19. The problem is that a negative test doesn’t mean you don’t have it. In fact, there are limited data on the accuracy (or sensitivity) of PCR for this virus. In China, a small number of patients with clinically compatible illness were tested using PCR and it correctly identified as many as 72 percent and as few as 32 percent and was highly variable in repeat tests. For similar viral testing sensitivity runs at 50-70 percent correct positives.
What is most important is that this means between 30-50 percent of those tested are released back into the community when they are in reality infected.
This is made worse because mostly we just test those with obvious symptoms. It means we won’t catch any of those without symptoms – those we most need to catch. It’s likely we have large numbers of asymptomatic people already in the community unintentionally infecting many others. Data from Iceland show that this might be as high as 50 percent of cases.
Second, we haven’t and don’t have the capacity to do the accurate level of massive population testing we need to. Simple as that.
Third, even if the above were both 100 percent, we cannot tell if you have already been infected and recovered. We need antibody testing to become available for this to be known. This hopefully comes to NZ soon. Eventually it will and we will really know the true numbers of infections. This means we can calculate the all-important “case fatality rate” which is the key number to decode how to react to a pandemic. We really must know how lethal this virus is, and for who, compared to something we already know like the seasonal flu.
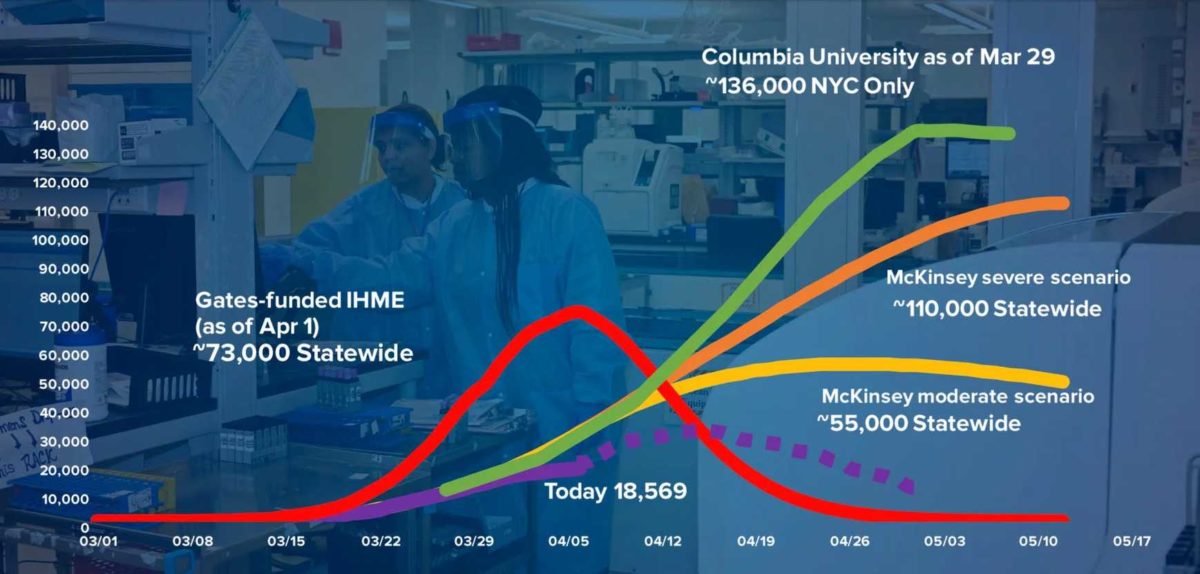
To be clear, we don’t know this number with any certainty, and the modelling used to predict deaths, and therefore government responses, depends on this as yet uncertain number. The WHO’s original estimate was 3.4 percent, with the latest estimates looking closer to 0.3 percent and has usually come down further with more accurate measurement in other pandemics. The figures are still very uncertain. Seasonal flu has a case fatality rate of 0.1 percent.
I got most interested in this three weeks ago when I became sick with a sore throat, swollen glands, which eventually changed to a dry cough, difficulty breathing especially at night time, and then a lung infection. Repeated calls to the Healthline and my doctor resulted in vague advice not to worry and “drink more fluids”. Everyone in my house ended up with symptoms, all less severe than me. This really piqued my interest in how we were missing the boat. I had travelled on aircraft and mixed with people from overseas (at Ironman NZ in Taupo). Yet, I was outside of scope for being tested.
Did I, and my family, have Covid-19? I don’t know, and that’s the point.
We were originally on a plan to “flatten the curve”. This means reduce the speed of infection, also called mitigation. This seems prudent given we know we have a potentially lethal virus circulating in our community, with no easy way to accurately detect it. As well, there are probably large numbers of asymptomatic people spreading. Mitigation aims to lessen the potential high demands on the health system so we can give those who need it the best quality of care.
To me, it seems most likely that we cannot contain this because we can’t measure it.
Yet, somewhere in the last week the strategy changed to an eradication policy. Even if full eradication isn’t the goal, if it’s just “seriously flattening the curve” that requires much wider, more accurate surveillance and then quarantine than we have.
Our current strategy has so many questions, but very few answers.
What’s the exit strategy for this eradication policy? When do we go back to work, how do we decide with reliable data, and what then? What do we do if we get more infections again? Do we go back to lockdown? What if we are not successful?
Do we just “try harder” and lock down more? When do we decide to give up and try something else? How much harm is done to health from economic collapse and poverty will we get? How compliant will New Zealanders be in the longer-term? Even a small amount of civil disobedience is essentially unenforceable?
In the end, the goal in public health is to get the best possible outcomes, for the least possible harm, with the tools and resources we have available now. So as more and more data emerge, and we see where we are at we must be willing and able to change our mind, and move in ways that maximise the best health outcomes and the least harms.
Given we currently have no way of identifying accurately enough who has this virus, especially asymptomatic positives, then mitigation is the most logical pathway, especially given the unknown and potentially large harms of extended lockdown. Let’s explore our Plan B. Now is good.